Disclaimer: The information provided in this article is for general informational purposes only and should not be considered legal, medical, or financial advice. While we strive to ensure accuracy, healthcare credentialing requirements may vary by provider, payer, and jurisdiction. Readers should consult qualified professionals or relevant authorities for guidance specific to their situation.
Starting a medical practice or joining a new healthcare organization should be an exciting step for any provider. However, before physicians can treat patients and be paid by insurance companies, they must complete a process known as provider enrollment.
Unfortunately, this process is rarely simple.
Paperwork, verification, payer communication, and strict compliance rules can quickly make the whole process quite stressful.
This is where healthcare credentialing services make a real difference. They help providers with their utmost services, including speeding enrollment, reducing administrative headaches, and allowing physicians to focus on patient care instead of paperwork.
Have questions about this story?
Ask Tundra for more details, context, or updates.
Understanding the Provider Enrollment Process
Provider enrollment is the process by which physicians, clinics, and other healthcare professionals are enrolled by insurance firms to enable payment for their services. The Centers for Medicare & Medicaid Services (CMS) explains that healthcare providers must complete an official enrollment process before they can bill Medicare or other insurance programs for services they deliver.
Insurance payers typically require providers to submit detailed information about their education, licenses, certifications, work experience, and malpractice insurance as part of the enrollment process.
The issue is that each payer has its own rules, forms, and timeline. One lost document or minor error may slow down the process for weeks or months.
For a new provider, such a delay means that patients may still receive care, but claims cannot be reimbursed during that period.
Credentialing and enrollment specialists help simplify this process by organizing provider data, preparing applications, reviewing documents for accuracy, and communicating with insurance payers to keep the enrollment moving forward.
Why Credentialing Delays Can Hurt Medical Practices
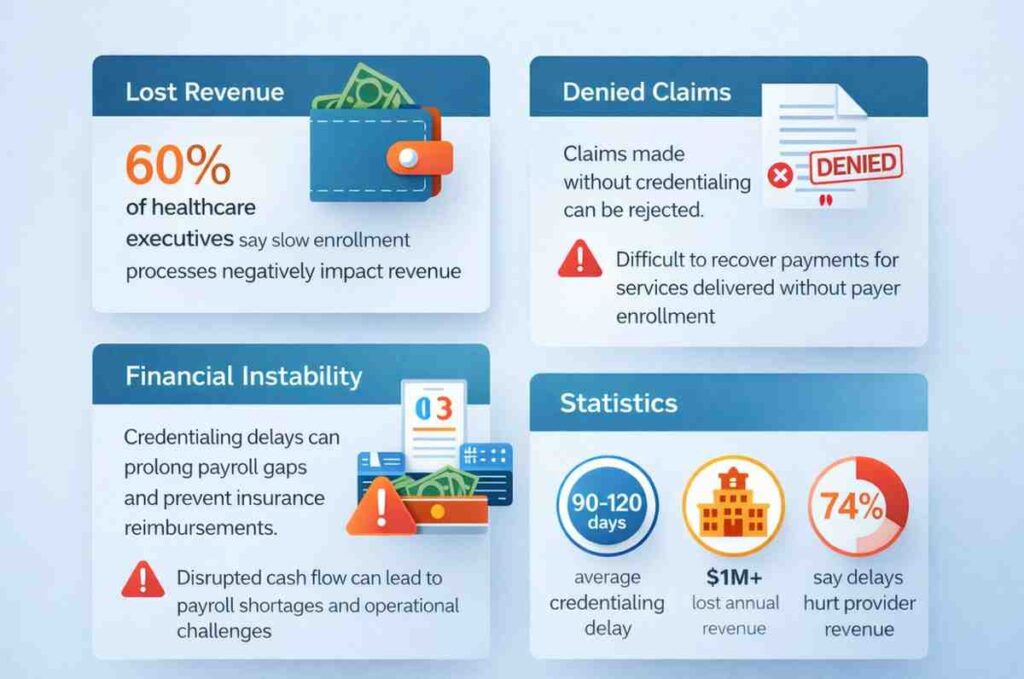
Most medical practitioners do not take credentialing delays seriously. If enrollment is not completed on time, providers may experience a disruption to their revenue, which can affect payroll, operating costs, and overall financial stability. In fact, survey data shows that 60% of healthcare executives report slow enrollment processes as having a negative impact on revenue.
If enrollment is not completed on time, providers may experience a disruption to their revenue. This may affect payroll, operating costs, and financial stability.
Sometimes, physicians begin treating patients without payer provision. If claims are made without appropriate enrollment, insurance companies can deny them. Getting those payments back may be highly challenging.
Healthcare credentialing services can help avoid such cases by ensuring applications are completed properly first. They also monitor payer feedback and keep on track to prevent unwarranted delays.
The Role of Organized Documentation
Documentation is also a major component of effective credentialing.
Payers need regular documents that contain license verification, board certification, professional references, and employment history.
The documents are usually lost or become obsolete when providers attempt to maintain these records independently.
Credentialing professionals ensure provider records are well-organized so all information is available whenever a payer asks them to verify.
When credentialing and billing procedures are coordinated correctly, claims flow more smoothly through payer systems.
How Credentialing Services Reduce Administrative Burden
Being a healthcare practitioner comes with numerous duties in itself. Doctors need to be concerned with the patient, clinical paperwork, and treatment choices. Administrative processes such as enrolment paperwork may consume hours of productive time.
These time-consuming tasks are transferred to healthcare credentialing services, where their teams handle application submissions, record-keeping compliance, and payer contact.
For busy practices, this support improves both efficiency and job satisfaction.
Keeping Up with Changing Healthcare Regulations
The healthcare rules are shifting a lot, particularly regarding insurance policies and compliance guidelines. Payers or regulatory agencies may revise credentialing requirements that were acceptable last year.
Professional credentialing teams stay informed about these changes. They are well-informed about payer policies, federal requirements, and documentation standards that providers should meet.
Because credentialing is closely linked with medical billing and coding, compliance in both areas becomes easier when experienced professionals manage the process. Proper enrollment also guarantees that the billing teams can make claims without any regulatory hassle.
Improving Revenue Stability Through Proper Enrollment
Credentialing is not only an administrative requirement but also a significant element of financial security within healthcare organizations.
In cases where providers are correctly enrolled with insurance networks, claims can be processed quickly and reimbursements made promptly.
Even perfectly documented claims can be dismissed without proper enrollment.
This results in payment delays and additional workload for billing personnel who must resubmit or appeal claims.
Why do many practices choose Professional Credentialing Support?
Many modern healthcare practices choose to work with credentialing specialists, but the process has become more complex over time. Insurance companies now require detailed verification steps and strict documentation standards.
Credentialing professionals understand payer expectations and navigate the system efficiently. Their experience helps avoid common errors that slow down approvals.
Final Thoughts
Provider enrollment should not feel like an obstacle for healthcare professionals who want to focus on patient care. With proper support, the process becomes manageable and much less stressful.
Healthcare credentialing services simplify enrollment by organizing documentation, communicating with insurance payers, and ensuring all requirements are met. This structured approach not only speeds up approvals but also strengthens the foundation for smooth billing operations.
For providers who want to avoid delays, reduce administrative pressure, and maintain consistent reimbursements, professional credentialing support is a practical and valuable solution.










